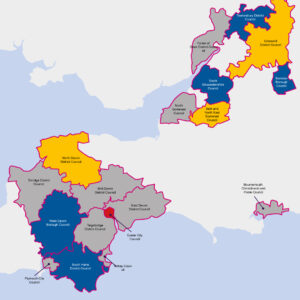
Election 2024: South West political preview
Labour have won the Kingswood Parliamentary Constituency for the first time since 2005 in a hotly contested by-election caused by the resignation of former MP Chris Skidmore.

Labour have won the Kingswood Parliamentary Constituency for the first time since 2005 in a hotly contested by-election caused by the resignation of former MP Chris Skidmore.

Britain has made remarkable progress since Boris Johnson promised to invest £5 billion through the Project Gigabit programme. This ambitious scheme aimed to provide all,

Date Added: 07 March 2024Closing Date: 28 March 2024 Job Title: Account Manager Working For: JBP Associates Location: Bristol Salary: Competitive Length of Contract: Permanent

Discover how the Government’s £6 billion fund aims to tackle the housing crisis, offering hope for affordable housing solutions.

Rural Economy: Explore key insights into revitalizing rural areas, fostering growth, and addressing economic challenges.

Date Added: 16 February 2024Closing Date: 16 March 2024 Job Title: Junior Designer Working For: JBP Associates Location: Bristol Salary: £23,000 – £28,000 Length of

Labour have won the Kingswood Parliamentary Constituency for the first time since 2005 in a hotly contested by-election caused by the resignation of former MP Chris Skidmore.

In the swiftly evolving landscape of B2B communications, including the logistics sector, adapting strategies is crucial to staying relevant. Chris Lawrance, Managing Director at JBP, emphasizes the necessity for logistics PR teams to revamp their approach. He outlines six key actions for 2024:
Understand the broader business potential of communication strategies.
Prioritize digital proficiency for future engagement plans.
Integrate PR and Search Engine Optimization for enhanced ROI.
Harness the power of B2B influencer programs.
Embrace a human and responsible approach.
Explore the value AI can bring to communication efforts.

Date Added: 3 February 2024Closing Date: 29 February 2024 Job Title: Account Executive Working For: JBP Associates Location: London Salary: £27,500 Length of Contract: Permanent